Also known as
Pemphigus vulgaris or PV
Description
- The immune system consists of white blood cells and Proteins known as antibodies that protect the body against foreign invaders (virus and bacterial infections), cancer, and poisons or toxins. In autoimmune conditions such as Pemphigus, the immune system, for no known reason, launches an attack against the body. In Pemphigus, the epithelial cells (the first layer) of skin and the mucous membrane (lining of the mouth) are attacked.
Symptoms
- Mouth or oral blisters or sores appear weeks or months before skin lesions.
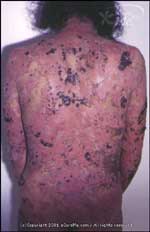
- Lesions start in the scalp, upper trunk, and chest or back, and extend to under arms, face, and the groin area (between legs).
- Lesions and sores have a red base and appear in a variety of shapes with irregular borders.
- Bullae or fluid-filled thin sacs are seen on the skin surface.
- Bullae may rupture after one to two days
- Shallow erosions are scattered throughout, and heal very slowly, and the area is often not scarred after healing, but may be darker than surrounding skin.
- Blisters (small fluid-filled sacs on the skin or inside the mouth) appear mainly on the back and easily break, with the underlying base forming a crusty shallow sore or ulcer that takes months to heal.
- The outer layer of the skin can easily be peeled or rubbed off, and pressure on the sides of the blister causes it to extend further underneath the skin (i.e., Nikolsky’s sign).
- The disease can be fatal if left untreated.
Cause
- Auto-immune:
– PV-antibodies (IgG) in the blood attack a certain protein in the skin or mouth that, under normal conditions, help to bind the epithelial cells and the skin together. When the bond between these cells is destroyed, blistering lesions and sores form in the mouth or skin.
- Genetics:
– Certain groups with abnormal genes may be more prone to develop PV and other autoimmune disorders.
How the diagnosis is made
- History:
-
- Symptoms
- Medications
- Illnesses
- Allergies
- Family history
- Habits
- Surgeries
- Vaccination history
- Medical exam:
-
- Entire body
- Skin — blisters, bullae, Nikolsky’s sign
- Scalp and mouth
- Blood tests for the number and type of white blood cells, auto-antibody levels, or titers (IgG)
- Lesions may be scraped or biopsied and sent to the laboratory for examination under microscope that will show the presence of IgG and C3 Proteins in between epithelial cells. If infection is suspected, scrapings and fluids from blisters can be examined by a microbiologist, who looks for the presence of bacteria.
- A urine sample for analysis may be needed.
- Chest X-Rays may be done in elderly patient.
Risk Factors
- Males = Females
- Age: 30 – 60 range
- Presence of HLA-A10, HLA-DR4, and HLA-DRW6 antigens (Proteins on the epithelial cell surface).
- Race:
– Mediterranean and Jewish descent
- Medications:
- Penicillamine
- Capoten
- Feldene
- Rifampin
- Phenobarbital
-
- Penicillin
Treatment
- This is not contagious.
- Depends on severity of illness
- May need admission to the hospital
- Food may be chopped, liquid, or pureed if the mouth lesions are painful.
- Isolation from other patients may be needed so that the lesions do not get contaminated or infected.
- Nurses soak lesions and remove crusts
- Wrap gauze around the lesions so that they do not leak.
- Replace fluids if patient dehydrated
- Antibiotics intravenously or through the veins (IV) if lesions are infected
- Tylenol or other painkillers (analgesic) may be used.
- Benadryl solution or Dyclonine candy (for kids) can help with mouth pain.
- Xylocaine is a topical analgesic often used.
- Immune system suppressants (i.e., weaken the immune attack):
– Steroids such as Prednisone by mouth (IV if cannot swallow) is started right away and continued for life. Side effects include thinning of the bones, stomach ulcers, or bleeding and infection. Cyclophosphamide, Azathioprine, Cyclosporine, gold, and other drugs are much stronger, but also have more severe side effects.
- Plasmapheresis is a technique that filters the plasma portion of the blood and removes IgG.
- Therapies may be combined and used together.
If You Suspect this Condition
- Contact your doctor immediately. He may then consult with an immunologist and start treatment.
Similar Conditions
- Infections: